This can feel abrupt, almost overnight. Yet biologically, these changes have been building quietly for years. Skin often reacts before menopause is named, because it is densely packed with hormone receptors and depends on them to maintain its structure. When those signals weaken, the effects surface where they are easiest to feel.
What follows isn’t a cosmetic inconvenience. It’s a functional change in the body’s largest organ—and one that deserves to be understood on its own terms.
Key Takeaways (For When You Are Skimming Between Meetings)
- Menopause creates barrier dysfunction, not just surface dryness – The stratum corneum’s lipid structure fundamentally changes when estrogen declines.
- 60%+ of women experience noticeable skin changes during the menopausal transition – You’re not alone, and it’s not poor skincare discipline.
- Ceramides shorten and decrease, creating gaps that allow water to escape even when skin looks intact (the “thinning mortar” problem).
- Traditional moisturizers fail because they assume an intact barrier – Humectants pull from depleted stores, occlusives sit on disorganized surfaces.
- Recovery takes longer in estrogen-deficient skin – Daily stressors accumulate because repair mechanisms slow significantly.
- Ethnicity affects baseline characteristics and menopausal response – One-size-fits-all approaches miss important biological variation.
- Progress comes in quiet increments – Fewer flare-ups, less night itching, more predictable skin (not instant radiance). For many women, the first sign that something in the body is shifting isn’t a missed period or a hot flush. It’s skin that suddenly feels unfamiliar. A face that tightens by mid-afternoon. Legs that itch for no obvious reason. A favourite moisturiser that used to be enough, now absorbed and forgotten within minutes.
In this article
- Midlife Skin Is Not Passive—Here’s What’s Actually Happening
- Why “Skin Ageing” Alone Doesn’t Explain Midlife Skin Changes
- The Barrier Problem Beneath the Symptoms
- Why Moisturiser Relief Is Often Short-Lived
- Recovery Takes Longer—and That Changes Expectations
- What Skin Actually Needs Now
- Ethnicity Adds Another Layer of Complexity
- Living With Skin That Is Changing, Not Failing
Midlife Skin Is Not Passive—Here’s What’s Actually Happening
Skin is often described as a surface, but it behaves more like a living system. It regulates temperature, keeps irritants out, manages water balance, and communicates with the immune and nervous systems. Every one of those roles depends on tightly coordinated biological processes.
By midlife, several influences converge at once. Hormone signalling within the skin begins to decline during perimenopause, even while cycles are still regular. Systemic levels of estrogen, progesterone, and androgens gradually fall. At the same time, everyday factors—cleansing habits, indoor heating, sun exposure, stress—continue to place demands on a system that is becoming less resilient.
This helps explain a common frustration: you haven’t changed anything, yet your skin behaves as if you have. The routine that worked for years now feels unreliable, and the problem doesn’t resolve with more effort or better compliance.
Why “Skin Ageing” Alone Doesn’t Explain Midlife Skin Changes
Chronological ageing does affect skin, but midlife skin change follows a different pattern. Research shows that sex hormones play a distinct role in how skin maintains its barrier, produces lipids, regulates inflammation, and repairs itself after stress.
These shifts often begin subtly. Early dryness or sensitivity may be easy to dismiss, especially when it comes and goes. Over time, though, the cumulative effects become harder to ignore. The skin feels thinner, less elastic, slower to recover. Lines appear more quickly after dehydration. Pigment lingers longer after sun exposure or irritation.
The timing matters. Many of these changes accelerate during the menopausal transition, not simply with age. That distinction is important, because it explains why the experience can feel disproportionate—and why standard advice often falls short.

How Common These Changes Really Are
Large studies of perimenopausal and postmenopausal women show how widespread these experiences are:
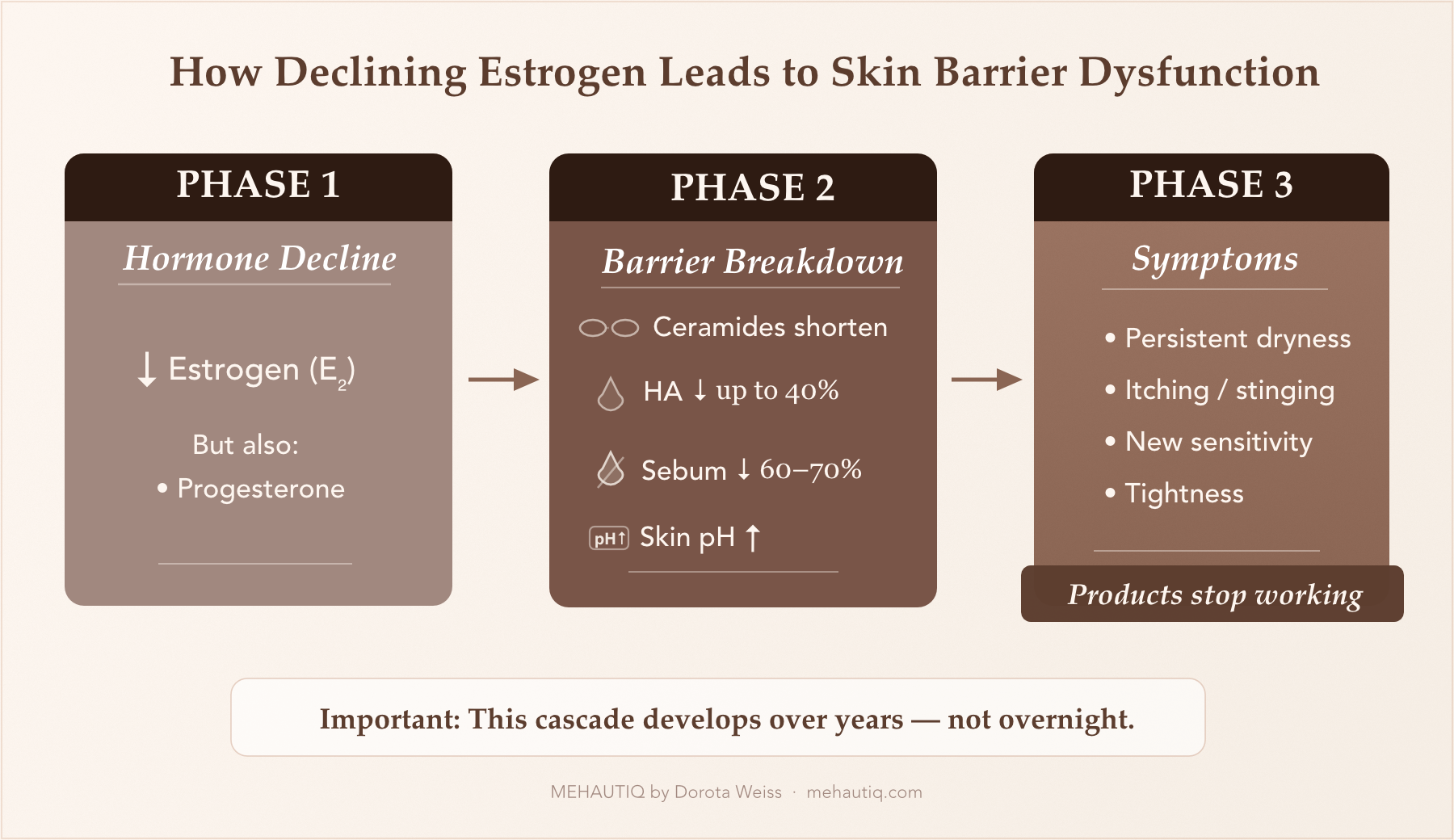
- Over 60% report noticeable skin changes during the menopausal transition.
- 64% describe persistent dryness.
- 56% report itching, stinging, or crawling sensations.
Dryness rarely stays confined to one area. While the face draws attention first, many women notice it on the arms, legs, or torso—often alongside new sensitivity to fabrics, weather, or products that were once unproblematic.
Itching deserves special mention. In estrogen-deficient skin, nerve endings become more reactive and histamine release increases. That low-level irritation can create a background discomfort that’s hard to name but difficult to ignore, especially at night.
If this sounds familiar, it isn’t a failure of skincare discipline. It’s a predictable response to biological change.
The Barrier Problem Beneath the Symptoms
The outermost layer of skin—the stratum corneum—acts as a barrier that controls water loss and blocks irritants. It’s often compared to a brick wall: flattened skin cells are the bricks, and lipids fill the spaces between them, forming a seal.
Those lipids are not optional extras. They are carefully organised sheets made from ceramides, cholesterol, and free fatty acids. Together, they limit transepidermal water loss (TEWL), the slow evaporation of water from the skin surface.
During menopause, this structure changes in several ways at once.
Ceramides: Less, and Not the Same
Ceramides make up roughly half of the barrier’s lipid content. In postmenopausal skin, their levels drop—and the ceramides that remain are shorter in chain length. Shorter chains don’t interlock as effectively, leaving microscopic gaps that allow water to escape.
Think of it less as missing bricks and more as thinning mortar. The wall still stands, but it no longer seals properly. You can smooth the surface, but the underlying leak remains.
Research consistently links ceramide length and abundance to estrogen levels. When estrogen falls, barrier integrity weakens—even if the skin looks intact.
Hyaluronic Acid: A Smaller Reservoir
Hyaluronic acid binds water within the skin, helping maintain volume and flexibility. Estrogen stimulates its production. As levels decline, hyaluronic acid in the dermis can drop by up to 40%.
This matters because many hydrating products rely on existing water reserves. When those reserves shrink, drawing from them becomes less effective—sometimes counterproductive.
It’s similar to drawing water from a well that hasn’t been refilled. You can keep lowering the bucket, but eventually there’s little left to bring up.
Sebum: The Missing Top Layer
Sebum provides a natural occlusive film that slows evaporation. After menopause, sebum production falls by 60–70%, removing a layer of protection pre-menopausal skin took for granted.
Without it, the barrier must work harder with fewer resources. Products now have to compensate for both internal lipid loss and an absent surface seal.
pH and Enzyme Slowdown
Healthy skin is slightly acidic. That acidity allows enzymes to convert lipid precursors into the organised structures the barrier needs. After menopause, skin pH drifts upward.
Even small shifts matter. When the environment becomes less acidic, those enzymes slow down. Lipids may be present but poorly assembled, leaving the barrier functionally incomplete.
Why Moisturiser Relief Is Often Short-Lived
This is where many women get stuck in a cycle: apply moisturiser, feel brief comfort, reapply, repeat.
Traditional moisturisers are designed for skin with an intact barrier. They combine humectants to draw water, occlusives to slow evaporation, and emollients to smooth texture. In younger skin, that’s usually enough.
In menopausal skin, several mismatches appear:
- Occlusives sit on a disorganised surface. Without a stable lipid matrix, oils and waxes don’t integrate well. They form a film, then wear off.
- Humectants pull from depleted stores. When deeper water reserves are low, drawing moisture upward can leave skin feeling tight again within hours.
- Barrier repair lags behind hydration. Even when water content improves temporarily, repair mechanisms remain slow. Once the product dissipates, dryness returns.
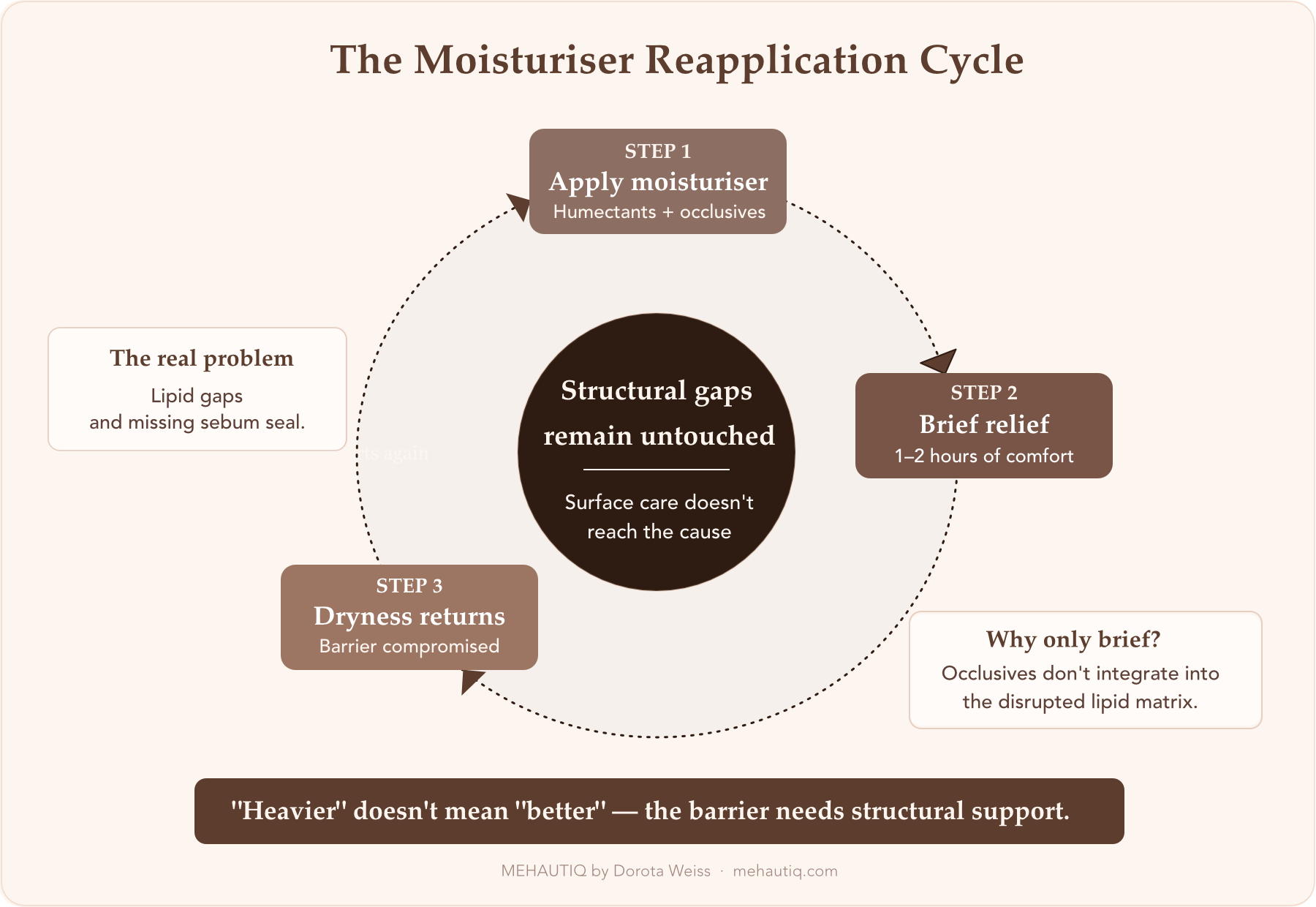

Laboratory studies show that in compromised barriers, heavy occlusion can even delay recovery. Skin repairs more effectively under conditions that allow some water movement—another reason “heavier” doesn’t always mean “better.”
This helps explain a familiar scene: standing in a shop aisle, comparing increasingly rich formulas, wondering why nothing seems to last.
Recovery Takes Longer—and That Changes Expectations
Barrier disruption happens easily in estrogen-deficient skin. Recovery takes longer.
When researchers deliberately disrupt the barrier and measure how quickly it repairs, postmenopausal skin lags significantly behind. Even when baseline dryness varies between individuals, repair speed consistently slows.
That delay means that daily stressors—cleansing, weather, friction—have a cumulative effect. The skin is still repairing yesterday’s damage when today’s arrives.
This doesn’t mean improvement is impossible. It does mean that comfort may come in increments rather than dramatic overnight change. Patience becomes part of the biology, not a personal virtue test.
What Skin Actually Needs Now
Effective support focuses less on surface sensation and more on restoring the barrier’s working parts.
Research points to several elements that matter most:
- Physiological lipid mixtures that resemble the skin’s own ratios, rather than generic oils.
- Long-chain ceramides, which interlock more effectively.
- pH-supporting ingredients that encourage proper lipid processing.
- Barrier-supportive actives such as niacinamide or panthenol, which support lipid synthesis and repair.
- Anti-inflammatory support, acknowledging the low-grade inflammation that accompanies hormone decline.
These approaches don’t create instant results. They aim to rebuild capacity, not just mask symptoms.
Importantly, evidence here is still evolving. Some long-term studies suggest that mismatched moisturisers may even slow endogenous repair. That uncertainty is part of why midlife skin care benefits from restraint as much as action.
Ethnicity Adds Another Layer of Complexity
Baseline barrier characteristics differ across ethnic groups—and menopause compounds those differences.
- African American skin often has strong structural cohesion but lower ceramide levels—up to 50% lower than Caucasian skin—making dryness more visible despite resilience.
- Asian skin tends to have higher lipid and water content but greater sensitivity to disruption.
- Caucasian skin typically falls between these patterns.
During menopause, ceramide depletion occurs across all groups, layering new deficits onto existing ones. This helps explain why dryness may present differently, and why routines that work for others don’t always translate.
The implication isn’t to categorise, but to personalise. Barrier biology isn’t uniform—and neither is response.
Living With Skin That Is Changing, Not Failing
Midlife skin changes aren’t a sign that something has gone wrong. They reflect a system adapting to a new hormonal environment with fewer resources and slower repair.
Understanding this shifts the emotional tone of care. Reapplication isn’t indulgence; it’s compensation. Sensitivity isn’t fragility; it’s altered signalling. The need for different support isn’t a regression—it’s context.
Progress here tends to be quiet. Fewer flare-ups. Less nightly itching. Skin that feels more predictable, even if not perfect.
For many women, that reliability matters more than radiance.
Literature
Core Comprehensive Reviews on Menopause and Skin
- Kendall AC, et al. Menopause induces changes to the stratum corneum ceramide profile that are prevented by hormone replacement therapy. Scientific Reports, 2022; 12:21715.
- Shah MG, Maibach HI. Skin aging and menopause: implications for treatment. American Journal of Clinical Dermatology, 2002; 3(2):107–117.
- EMJ Reviews. Managing menopausal skin: a clinician’s review. EMJ Dermatology, 2025.
- Brincat MP, et al. Menopause and the effects of hormone replacement therapy on skin aging: a short review. Gynecological and Reproductive Endocrinology & Metabolism, 2024.
- Man MQ, et al. Aging-associated alterations in epidermal function and their clinical significance. Aging (Albany NY), 2020; 12(6):5551–5565.
- Nikoletić ĐC, et al. Menopause, menstrual cycle, and skin barrier function. Skin Research and Technology, 2025; 31(7):e70203.
- NBI Health. How menopause destroys collagen. NBI Health, 2025.
- Brincat M, Moniz CF, Studd JWW, et al. Sex hormones and skin collagen content in postmenopausal women. British Medical Journal (Clinical Research Edition), 1983; 287(6402):1337–1338.
- Viscomi B, Muniz M, Sattler S. Managing menopausal skin changes: a narrative review of skin quality changes, their aesthetic impact, and the role of hormone replacement therapy. Journal of Cosmetic Dermatology, 2025; 24(S4).
- Caussin J, Gooris GS, Groenink HWW, Wiechers JW, Bouwstra JA. Interaction of lipophilic moisturizers on stratum corneum lipid domains in vitro and in vivo. Skin Pharmacology and Physiology, 2007; 20(4):175–186.
- Khunger N, Mehrotra K. Menopausal Acne – Challenges And Solutions. Int J Womens Health. 2019 Oct 29;11:555-567. doi: 10.2147/IJWH.S174292.
- Wu Y, Olivero JW, Zhen Y. Compromised skin barrier and sensitive skin in diverse populations. Journal of Drugs in Dermatology, 2021; 20(4):S17–S22.
