Your skin has reinvented itself many times. Different seasons. Different products. Pregnancy, pills, stress, travel. You adjusted, tweaked, and usually found a way back to “normal.”
This time feels different.
The routine that worked for years suddenly…doesn’t. Your face can look deflated and tight by lunchtime. A bump on your shin leaves a bruise that hangs around for weeks. Makeup sits in lines you did not remember having. And, just to add insult, deep breakouts appear along your jaw as if your skin time‑traveled back to age 16-without your consent.
You may have quietly decided this is your fault: too many late nights, the “wrong” serum, not enough discipline.
It is not your fault. It is your hormones.
Once you understand exactly how menopause changes your skin, three things shift at once: you stop blaming yourself, you stop chasing random “anti‑aging” fixes, and you start making decisions that actually match what your skin is going through now-not what it used to be like ten years ago.
Key Takeaways (For When You Are Skimming Between Meetings)
- Estrogen loss hits skin through a triple mechanism: your body makes less estrogen, your skin makes less locally, and your cells become less responsive to what is left.
- Collagen drops quickly and is tied to time since menopause: you lose about 30% of dermal collagen in the first five years after menopause, and roughly 2% per year after that.
- Skin barrier problems are structural, not just “dryness”: ceramides decline, hyaluronic acid production slows, and sebum falls by about 40%, which means water leaks out faster than any single moisturizer can fix.
- Multiple systems change at once: collagen and elastin, thickness, barrier function, oil production, pigmentation, wound healing, acne patterns, rosacea, and the microbiome all shift together.
- Your skin is not failing; it is responding logically to hormonal withdrawal: understanding the mechanisms turns “nothing works anymore” into a clear, stepwise strategy.
In this article
- The Skin–Hormone Connection Nobody Explained
- The Triple Hit: Why Estrogen Loss Feels So Dramatic
- Collagen Loss: The Structural Shift You Can Feel
- Why Skin Feels Thinner, More Fragile, And More Transparent
- Constant Dryness In Menopause: A Structural Barrier Problem
- Why Healing Now Feels Like A Slow‑Motion Replay
- The Plot Twist: Acne At 45, 50, Or Beyond
- When Every Old Sun Spot Shows Up At Once
- Rosacea: When Flushing, Hot Flashes, And Hormones Collide
- Your Skin’s Ecosystem Rebuilds Itself: The Microbiome Shift
- When The Antennae Age: Declining Hormone Receptors
- Connecting The Dots: Barrier, Collagen, Pigment, Sebum
- What This Means For Your Skincare And Treatment Decisions
- Your Individual Trajectory Through Menopausal Skin Change
The Skin–Hormone Connection Nobody Explained
Menopause is not just a date on a calendar. Biologically, it is the moment your ovaries retire from hormone production. The signal that has been steady for decades gradually becomes a flickering light, then a blackout.
That shutdown does not happen overnight. During perimenopause—the two to eight years before your final period—hormones behave like a radio station drifting in and out of tune. One month you get a clear signal, the next month it is full of static. Your skin reacts to every distortion in that signal.
Maybe you recognize some of this:
- A month where your skin suddenly looked great—glowy, calm, almost like before followed three weeks later by intense breakouts along your chin.
- Moisturizers that used to feel rich and satisfying now vanish in seconds, leaving your face tight and uncomfortable by mid‑morning.
- Products you tolerated for years now sting on contact or trigger redness.
Those swings are not you “doing something wrong.” They are your skin reporting back, in real time, on the hormonal turbulence happening under the surface.
Here is the part that rarely makes it into beauty conversations: your skin is not just passively reacting to hormones made elsewhere. Skin cells can produce hormones locally, convert them into active forms, and respond through dedicated receptors. It is a full endocrine organ in its own right. When the broader hormonal environment changes, your skin’s internal hormone economy changes with it.
The Triple Hit: Why Estrogen Loss Feels So Dramatic
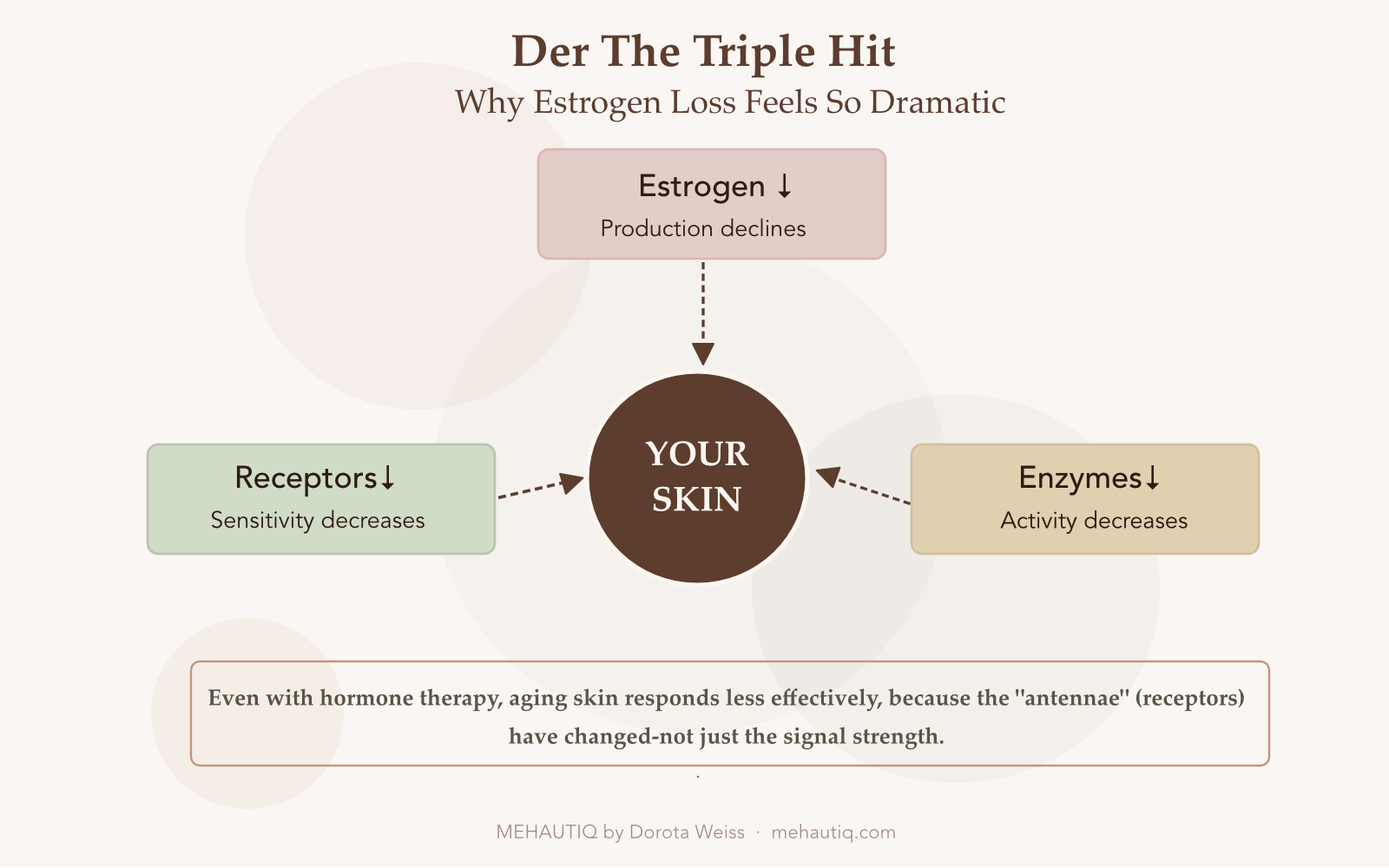
When estrogen declines, three distinct processes hit your skin at once:
- Circulating estrogen drops. This is the part everyone talks about: ovaries produce far less estrogen, so the hormone level in your bloodstream falls.
- Local estrogen production in the skin slows. Enzymes in your skin that once converted precursor hormones into estrogen become less active, so your skin’s “local supply” shrinks.
- Cellular receptors become less responsive. The receptors—think of them as antennae—that allow cells to “hear” estrogen’s message become less numerous or less sensitive over time.
Even if you could somehow hold estrogen levels at your 35‑year‑old baseline, aging skin would still respond less, simply because the antennae are not as good at picking up the signal.
This is why some women notice disappointing results from hormone replacement therapy (HRT) when it comes to skin: the issue is not just how much hormone is in circulation, but how well the skin can listen.
What this means for you:
- If your skin changed quickly around menopause, it is not “all in your head”—it is a triple withdrawal of signal, local support, and receptor sensitivity.
- Hormone therapy can help some aspects of skin aging, but it will not take skin back to “exactly like 25”, because the listening capacity of cells has changed.
- Focusing solely on adding more estrogen misses the bigger picture: supporting the structures and functions that are now under‑signaled (collagen, barrier lipids, wound healing, etc.).

Collagen Loss: The Structural Shift You Can Feel
Collagen is the scaffolding inside your skin. Type I is the sturdy framework (about 80% of dermal collagen), and Type III is the flexible mesh that gives skin its springiness. Together, they create that firm‑but‑bouncy feel people often call “youthful.”
After menopause, both types decline—and not gently.
- On average, about 30% of dermal collagen is lost in the first five years after menopause.
- Beyond that, collagen continues to decrease at roughly 2% per year.
- Long‑term studies suggest around 45% collagen loss 15 years after menopause in women who are not treated with hormone therapy.
Here is the twist that matters more than your passport age: collagen loss tracks more closely with time since menopause than with chronological age. A 60‑year‑old five years postmenopause can have less collagen than a 65‑year‑old just one year into menopause.
That is why you can feel like your face “suddenly dropped” around the time your period stopped, even if your actual birthday number did not change dramatically. The clock your skin is following is hormonal, not just chronological.
As collagen types shift, the ratio changes too. There is proportionally more loss of the “springy” Type III collagen, so skin does not just get looser—it also loses its ability to rebound.
You might notice:
- Smile lines that stay visible long after you have stopped smiling.
- Cheeks that fail the “pinch test”—when you gently pinch skin and it returns slowly instead of snapping back.
- The sense that your face has less internal “cushion,” even if your weight has not changed.
Why “collagen boosting” is only half the story
Inside your skin, there are two teams working on the collagen building:
- The construction crew: fibroblasts that make new collagen.
- The demolition crew: enzymes called matrix metalloproteinases (MMPs) that break down old or damaged collagen.
When estrogen is abundant, it keeps both teams in balance: fibroblasts are active, and MMPs are kept under control. When estrogen falls, that balance breaks.
- Fibroblasts receive fewer “build” signals and produce less new collagen.
- MMPs have less inhibition and break down collagen more aggressively.
It is like having half your builders laid off and your demolition crew told to speed up.
This is where many “collagen‑boosting” product may not work. Stimulating fibroblasts is useful, but if excess breakdown continues unchecked, it is like pouring more water into a bucket that still has a hole.
What this means for you:
- Expect faster structural changes in the first 5–10 years after menopause, not because you did something wrong, but because the biology is front‑loaded.
- Interventions that both stimulate new collagen and reduce excessive breakdown (some prescription retinoids, certain energy‑based devices, and medically supervised treatments) are more aligned with what your skin actually needs than generic “firming” products.
- Results will differ between women because baseline collagen, genetics, sun exposure history, and time since menopause all interact. Comparing your face to a same‑age friend’s is emotionally tempting—but biologically unfair.
Why Skin Feels Thinner, More Fragile, And More Transparent
Collagen is not the only structure changing. Overall skin thickness also declines.
Studies suggest that skin thickness drops by around 1.13% per year after menopause. That small yearly number compounds over time. Both the outer layer (epidermis) and deeper layer (dermis) become thinner. The wavy interface between them flattens. Elastic fibers degrade. The supporting fat and connective tissue under the skin lose volume.
In everyday life, this often shows up as:
- Bruises from minor bumps that would not have marked you ten years ago.
- Veins, tendons, and underlying structures becoming more visible on hands and face.
- Areas of “papery” skin that feel delicate and almost crêpe‑like.
Wound healing also slows. A biopsy site, scratch, or cosmetic procedure that used to settle within days can now take weeks to look calm again. That is not you “healing badly.” It is your skin working with a smaller structural toolkit.
What this means for you:
- When planning cosmetic procedures or dermatology treatments, it is realistic to budget 30-50% longer recovery time than timelines marketed to younger women.
- Gentle handling—both physically (less rubbing, tugging, over‑exfoliating) and procedurally (spacing treatments, avoiding stacking harsh interventions)—is not “being precious.” It is intelligent care for tissue that has less margin for error.
- Planning matters: avoid scheduling major skin procedures immediately before important events. Give your skin the extra time it now needs.
Constant Dryness In Menopause: A Structural Barrier Problem
Before menopause, your skin’s barrier works like well‑laid masonry: bricks (skin cells) held together by mortar (lipids such as ceramides, cholesterol, and fatty acids). Estrogen influences both the amount and organization of that mortar.
After estrogen drops, three key moisture‑related systems weaken:
- Barrier lipids (especially ceramides) decrease. The mortar between bricks becomes patchy and fragile, which allows water to escape more easily.
- Water‑binding molecules like hyaluronic acid decline. These molecules act like tiny sponges inside the skin, each capable of binding up to 1,000 times its weight in water. Fewer sponges mean less internal cushioning.
- Sebum (oil) production falls by about 40% in postmenopausal women. Unlike in men, where sebaceous activity remains more stable, women see a steady decline.
Put differently: you are losing the waterproofing mortar, the internal sponges, and the protective oil film-all at once.
You may see this as:
- Products absorbing instantly, with skin feeling tight again within hours.
- A “deflated” look, even when you are well hydrated and sleeping enough.
- Makeup clinging to dry patches or settling into lines, especially by afternoon.
- Winter or central heating becoming much harder to tolerate than before.
Layering more of the same moisturizer on top of a compromised barrier is like pouring water into a cracked vase. Until the cracks-the structural lipid gaps-are addressed, water will keep escaping.
What this means for you:
- You are not “high‑maintenance” for needing richer, more thoughtfully designed barrier care in your 40s and 50s. Your skin’s engineering has changed.
- Generic “anti‑aging” moisturizers designed for mildly dry, premenopausal skin often under‑deliver because they assume your barrier is still mostly intact.
- Strategies that combine ceramides, cholesterol, fatty acids, and water‑binding ingredients align better with what your skin is missing than light hydrators alone.
Why Healing Now Feels Like A Slow‑Motion Replay
Wound healing is one of the most estrogen‑sensitive processes in skin.
Estrogen influences:
- Inflammation: keeping it effective but controlled.
- Cell migration and proliferation: how quickly keratinocytes and fibroblasts move to fill a wound.
- Collagen deposition: building new supportive tissue in the wound bed.
- Remodeling: fine‑tuning the new tissue so it becomes stronger and more organized.
Remove or sharply reduce estrogen and every stage of this choreography slows.
That paper cut that used to be a three‑day non‑event can now stay noticeable for a week. A small procedure mark that formerly blended into your skin in ten days can stay pink for several weeks. Redness after peels or lasers may linger longer than expected.
For women on anti‑estrogen therapies (for example, certain breast cancer treatments), these changes can be even more pronounced, with higher rates of delayed healing and infection. On the flip side, controlled studies show that restoring estrogen-systemically or topically-can improve healing speed and quality in specific medical settings.
What this means for you:
- If you are peri‑ or postmenopausal, it is reasonable to assume slower recovery from any skin insult: procedures, injuries, even aggressive over‑the‑counter treatments.
- A “stronger” product is not automatically better. Supporting the barrier and avoiding excess irritation becomes a core strategy, not an optional extra.
- Always mention your menopausal status (and any hormone therapy) when discussing procedures with a dermatologist or surgeon; it can legitimately change how they plan your treatment and aftercare.
The Plot Twist: Acne At 45, 50, Or Beyond
One of the more emotionally loaded skin surprises during this life stage is acne that either appears for the first time or returns after decades.
This acne usually does not look like teenage acne. It often shows up as:
- Deep, painful papules or nodules along the jawline and chin.
- Fewer blackheads and whiteheads, more inflamed lesions.
- Spots that take longer to resolve and can leave persistent marks.
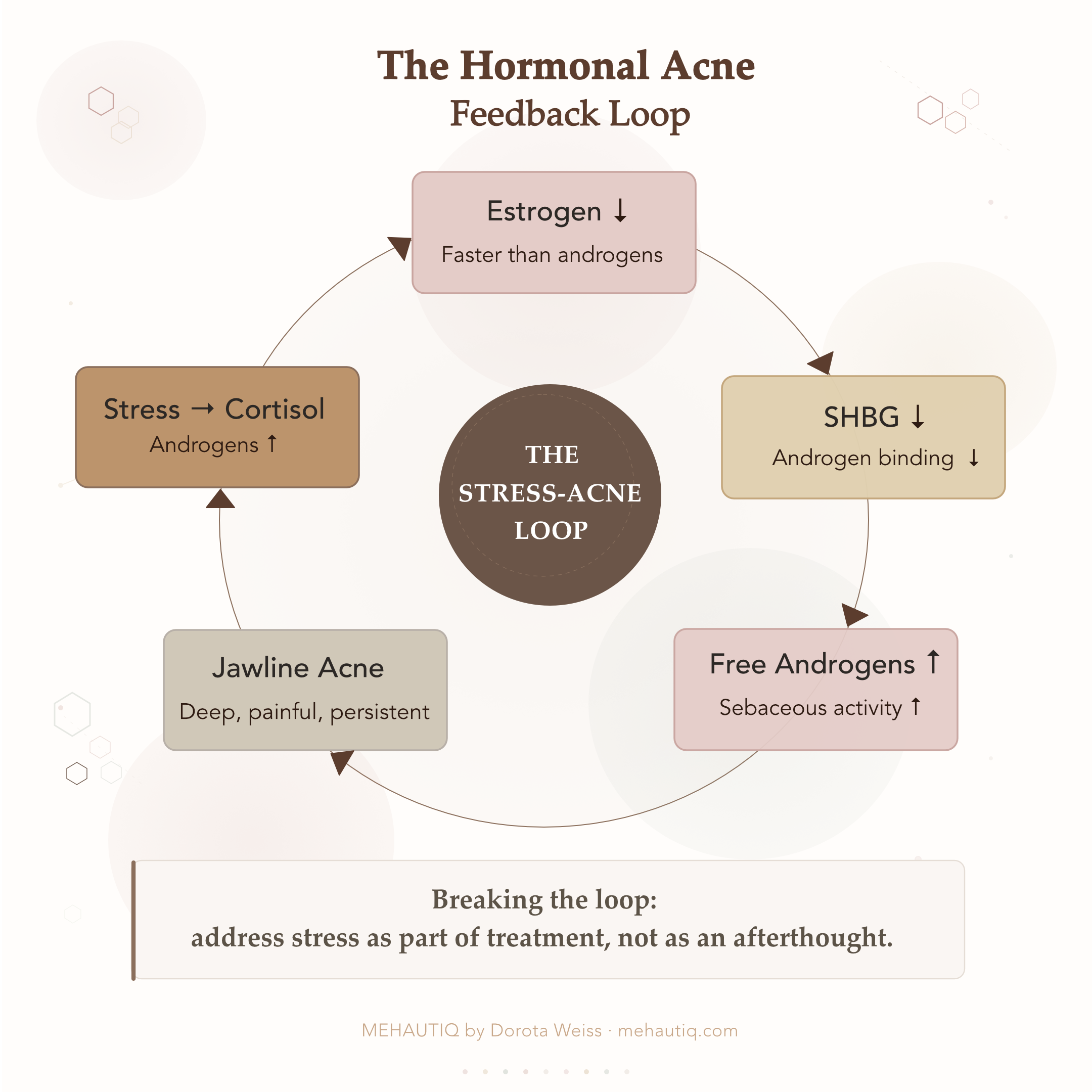
The hormonal driver is relative hyperandrogenism.
Here is what happens:
- Estrogen drops sharply.
- Androgen levels also fall, but more slowly.
- Levels of sex hormone‑binding globulin (SHBG)-a protein that binds testosterone and makes it less active-decrease.
The result: even if your absolute androgen levels are “normal,” a higher proportion is free and biologically active. Sebaceous glands, particularly around the lower face, become more sensitive to that androgen signal.
Complicating this, up to 60% of women with adult acne show evidence of increased androgen metabolites on urine testing, even when standard blood tests look normal. So a normal lab report does not always mean hormones are not involved.
Stress layers on top. Corticotropin‑releasing hormone (CRH), released during psychological stress, can push adrenal pathways toward more androgen production. The more stressed you feel about your skin, the more you may quietly fuel the exact biology driving breakouts-a cruel, very real loop.
What this means for you:
- If teenage regimens are not working on your 40s or 50s acne, it is because this is not teenage acne. Stripping cleansers, harsh scrubs, and aggressive over‑the‑counter spot treatments often do more barrier damage than good at this stage.
- Medical support (for example, with androgen‑modulating therapies or tailored topical regimens) is often appropriate rather than “overreacting.”
- Addressing stress is not fluffy advice. It is part of interrupting a hormonal feedback loop that genuinely influences your skin.

When Every Old Sun Spot Shows Up At Once
Pigment changes around menopause can be subtle or dramatic:
- New, scattered brown spots.
- Symmetric patches across cheeks, forehead, or upper lip (melasma).
- A general sense that the face looks more “blotchy” or weathered, even if you are diligent with SPF now.
Estrogen and progesterone both stimulate melanocytes, the cells that produce melanin. Pregnancy and birth control pills are classic triggers for melasma; menopause and hormone therapy can also nudge susceptible skin toward uneven pigmentation.
In practice, this often feels like:
- Sun damage that suddenly becomes visible, even if it was quietly building for years.
- Dark patches that resist standard brightening products.
- A sense that your complexion no longer looks “even,” no matter how carefully you care for it.
What this means for you:
- Sun protection is no longer optional or “when you remember.” It becomes a non‑negotiable baseline if you want to slow accumulating pigmentation during and after menopause.
- Hormonally influenced pigmentation is typically more stubborn than purely UV‑driven spots. Ingredients and treatments need to target multiple steps: melanin production, transfer, and turnover-not just one enzyme.
- Expect progress to be slower and more cyclical. Improvement may track with hormonal stability, treatment consistency, and-again-time since menopause.
Rosacea: When Flushing, Hot Flashes, And Hormones Collide
Rosacea often intensifies between 40 and 60, especially in women. For some, perimenopause is a perfect storm: hot flashes, vascular reactivity, and barrier vulnerability converge.
You might notice:
- Flushing episodes that are more frequent, more intense, and more easily triggered.
- A background redness that does not fully fade between flares.
- Previously effective treatments feeling less helpful.
Here is the paradox: population data suggest that overall rosacea prevalence is lower in postmenopausal women than in premenopausal women. In other words, the turbulent, fluctuating years can be your worst period—and then, as hormones stabilize after menopause, symptoms may ease.
Complicating matters, menopausal hormone therapy is associated with an increased risk of rosacea in some studies. So trading hot flashes for hormonal therapy can, in a subset of women, trade one kind of flushing for another.
What this means for you:
- If your rosacea feels out of control during perimenopause, that does not mean it will only get worse forever. The most chaotic window is often the transition, not the destination.
- Focusing on strict trigger management, gentle routines, and barrier repair during hormonal turbulence can help bridge you to a more stable postmenopausal phase.
- If you are considering or already on hormone therapy, it is worth a direct conversation with your dermatologist about how this might interact with rosacea—and how to monitor and manage it.
Your Skin’s Ecosystem Rebuilds Itself: The Microbiome Shift
Your skin hosts a living community of bacteria, fungi, and other microorganisms-the microbiome. This community helps train your immune system, influences inflammation, and contributes to barrier function.
After menopause, researchers see measurable shifts in this ecosystem:
- Bacteria that thrive in oilier environments (like some Cutibacterium species) become less abundant.
- Microbes that prefer drier conditions (such as certain Streptococcus species) increase.
- Overall diversity and balance can change in ways that are still being mapped.
One helpful way to picture this: menopause is like a neighborhood whose climate changed from mild and humid to colder and drier. The residents who liked humidity move out. New tenants who prefer dryness move in. The neighborhood is still a community-but it behaves differently.
You might experience this as:
- Products that suddenly sting or cause redness when they never did before.
- Breakouts or irritation in response to formulas that used to be safe “basics.”
- A vague sense that your skin has become “touchier” and less predictable.
The science here is still developing, and not every shift is fully understood. But the day‑to‑day message is already clear: your skin is not being dramatic; it is a different ecosystem now.
What this means for you:
- Routines that served you well in your 30s were designed for a different microbiome and oil profile. Updating products is not vanity—it is adaptation.
- Harsh cleansers, frequent scrubs, and over‑use of strong actives can destabilize this already‑shifting ecosystem further. Think “support and balance,” not “scrub into submission.”
- Claims about “resetting” or “perfecting” the microbiome are, at this stage, ahead of the evidence. What is supported is gentler care, avoiding unnecessary disruption, and respecting that your skin’s community is changing with you.
When The Antennae Age: Declining Hormone Receptors
Hormones need receptors to exert their effects. In skin, estrogen receptors (ERα and ERβ) sit on keratinocytes, fibroblasts, melanocytes, and blood vessel cells. Early in life, both men and women have similar levels of these receptors.
With age, especially after around 70, ERβ expression in epidermal cells declines. Even before that point, receptor dynamics change.
A useful analogy: think of estrogen receptors as Wi‑Fi receivers in a house. In your 30s, you have strong routers in every room, and the signal is clear. As you age, some routers are removed, and others lose range. Even if you upgrade your internet plan (more estrogen), the connection in distant rooms (aging skin areas) will not feel as strong as it once did.
This is part of why identical hormone levels can produce very different skin responses at 45, 60, and 75.
What this means for you:
- There is a biological limit to how much any hormone‑directed approach can rewind skin changes. This is not pessimism; it is realistic expectation‑setting.
- The priority gradually shifts from “reversal at all costs” to preservation and prevention: protecting remaining collagen, maintaining barrier integrity, and avoiding unnecessary damage.
- When comparing options (from hormone therapy to topical actives and procedures), it helps to ask: “Is this supporting what my skin can still do?” rather than “Will this make me look like I did at 28?”
Connecting The Dots: Barrier, Collagen, Pigment, Sebum
When you zoom out, the picture becomes clearer:
- Collagen drops by about 30% in the first five years after menopause, and continues to decline.
- Skin thickness decreases by a little over 1% per year.
- Sebum production falls by around 40%.
- Ceramide profiles shift.
- Hyaluronic acid production slows.
- Wound healing is delayed.
- Pigmentation patterns change.
- Acne can emerge or worsen.
- Rosacea can flare with hormonal turbulence.
- The microbiome reorganizes.
- Receptor sensitivity declines over time.
These are not separate, random events. They are different faces of one core reality: estrogen withdrawal in a biologically active organ.
Generic “anti‑aging” messaging often treats each issue as isolated-wrinkles here, dryness there, spots somewhere else. That framing makes you feel like you are constantly playing whack‑a‑mole with serums and treatments.
Seeing these changes as interconnected allows for a more coherent strategy.
| System | Change | Timeline | Impact |
|---|---|---|---|
| Collagen | 30% loss | First 5 years postmenopause | Lines deepen, skin sags, firmness decreases |
| Elastin | Fiber degradation | Progressive throughout menopause | Skin doesn’t bounce back, slower recovery |
| Barrier | Ceramide/ HA/ Sebum decline | Begins perimenopause, accelerates postmenopause | Chronic dryness, sensitivity, irritation |
| Thickness | 1.13% annual loss | Continuous postmenopause | Fragility, translucency, visible vessels |
| Healing | Delayed repair mechanisms | Immediate at menopause onset | Longer recovery, persistent redness |
| Hormonal Balance | Relative hyperandrogenism | Variable during perimenopause | Adult acne, localized oiliness |
| Pigmentation | Melanocyte hyperactivity | Triggered by hormonal fluctuation | Uneven tone, age spots |
| Microbiome | Ecosystem reorganisation | Follows sebum changes | Product sensitivities, altered barrier function |
What This Means For Your Skincare And Treatment Decisions
Instead of asking “What product should I buy now?”, a more powerful set of questions in your 40s and 50s is:
Which systems in my skin are under the most pressure right now?
- Structural (collagen, elastin, thickness)?
- Barrier (ceramides, lipids, water‑binding molecules)?
- Oil balance (dryness with local oiliness or acne)?
- Inflammation and healing (rosacea, sensitivity, slow recovery)?
- Pigmentation?
Where do I see the biggest gap between what my skin is doing and what my life currently demands?
- Frequent public‑facing work and not enough time for visible downtime after procedures?
- Caring responsibilities that limit elaborate routines?
- High stress, poor sleep, and little margin for irritation?
From there, your strategy becomes less about chasing the next trend and more about aligning interventions with biology:
- Barrier dysfunction calls for targeted lipid support and gentle routines, not just “more moisturizer.”
- Collagen loss calls for approaches that both encourage new formation and temper excessive breakdown, within the limits of your risk tolerance, recovery capacity, and medical guidance.
- Dryness calls for water‑binding molecules plus structural repair and appropriate occlusion, not just misting more often.
- Adult acne calls for hormonal thinking and stress awareness, not just recycling teenage acne kits.
- Slower healing calls for respectful planning-longer recovery windows, fewer overlapping irritants, and honest conversations with practitioners.
Your Individual Trajectory Through Menopausal Skin Change
Two women can be the same age, hit menopause in the same year, and live in the same city-and their skin journeys can look completely different.
Genetics, lifetime sun exposure, smoking history, nutrition, stress, underlying health, medication, and age at menopause all influence how the mechanisms described here play out on a real human face.
There is no “correct” way for menopausal skin to look.
There is only:
- What your skin is showing you right now.
- What matters most to you in this life stage (comfort, confidence, simplicity, discretion, experimentation, or some combination).
- Which levers-medical, cosmetic, behavioral-you are willing and able to pull.
The most important shift is this: moving from self‑blame and random trial‑and‑error to informed, compassionately realistic strategy.
Your skin is not misbehaving. It is speaking a hormonal language. Now that you understand the grammar and vocabulary of that language-collagen loss timelines, barrier changes, sebum decline, healing shifts, microbiome turnover-you can start responding in kind.
Not with panic.
With precision.
With patience.
And with the grounded confidence that comes from knowing: your skin is not failing. It is adapting. You get to adapt with it.
Literature
Core Comprehensive Reviews on Menopause and Skin
- Thornton MJ. Estrogens and aging skin. Dermatoendocrinol. 2013 Apr 1;5(2):264-70. doi: 10.4161/derm.23872.
- Brincat MP et al. Managing Menopausal Skin Changes: A Narrative Review. Journal of Cosmetic Dermatology, 2024, doi/10.1111/jocd.70393.
- Kamp E, Ashraf M, Musbahi E, DeGiovanni C. Menopause, skin and common dermatoses. Part 2: skin disorders. Clin Exp Dermatol. 2022 Dec;47(12):2117-2122. doi: 10.1111/ced.15308.
- Rzepecki AK, Murase JE, Juran R, Fabi SG, McLellan BN, Estrogen-deficient skin: The role of topical therapy, International Journal of Women’s Dermatology, Volume 5, Issue 2, 2019, https://doi.org/10.1016/j.ijwd.2019.01.001
- Brincat M.,Pollacco J., Menopause and the effects of Hormone Replacement Therapy on skin aging: A Short Review, GREM Gynecological and Reproductive Endocrinology & Metabolism (2024); Volume 5 – 1/2024:034-037 doi: 10.53260/grem.2450106.
- Zomer HD, Cooke PS. Targeting estrogen signaling and biosynthesis for aged skin repair. Front Physiol. 2023 Oct 31;14:1281071. doi: 10.3389/fphys.2023.1281071.
- Reilly DM, Lozano J. Skin collagen through the lifestages: importance for skin health and beauty. Plast Aesthet Res. 2021;8:2. http://dx.doi.org/10.20517/2347-9264.2020.153.
- Reus TL, Brohem CA, Schuck DC, Lorencini M, Revisiting the effects of menopause on the skin: Functional changes, clinical studies, in vitro models and therapeutic alternatives, Mechanisms of Ageing and Development, Volume 185, 2020, 111193, https://doi.org/10.1016/j.mad.2019.111193.
- Kendall AC, Pilkington SM, Wray JR, Newton VL, Griffiths CEM, Bell M, Watson REB, Nicolaou A. Menopause induces changes to the stratum corneum ceramide profile, which are prevented by hormone replacement therapy. Sci Rep. 2022 Dec 15;12(1):21715. doi: 10.1038/s41598-022-26095-0.
- Murphy B, Grimshaw S, Hoptroff,M et al. Alteration of barrier properties, stratum corneum ceramides and microbiome composition in response to lotion application on cosmetic dry skin. Sci Rep 12, 5223 (2022). https://doi.org/10.1038/s41598-022-09231-8.
- Khunger N, Mehrotra K. Menopausal Acne – Challenges And Solutions. Int J Womens Health. 2019 Oct 29;11:555-567. doi: 10.2147/IJWH.S174292.
- Dias da Rocha MA, Saint Aroman M, Mengeaud V, Carballido F, Doat G, Coutinho A, Bagatin E. Unveiling the Nuances of Adult Female Acne: A Comprehensive Exploration of Epidemiology, Treatment Modalities, Dermocosmetics, and the Menopausal Influence. Int J Womens Health. 2024;16:663-678, https://doi.org/10.2147/IJWH.S431523.
- Bagatin E, Freitas THP, Rivitti-Machado MC, Machado MCR, Ribeiro BM, Nunes S, Rocha MADD. Adult female acne: a guide to clinical practice. An Bras Dermatol. 2019 Jan-Feb;94(1):62-75. doi: 10.1590/abd1806-4841.20198203. Erratum in: An Bras Dermatol. 2019 Mar-Apr;94(2):255. doi: 10.1590/abd1806-4841.2019940202.
- Yang F, Wang L, Jiang X. Clinical characteristics of rosacea in perimenopausal women. Skin Res Technol. 2024 Jan;30(1):e13542. doi: 10.1111/srt.13542.
- Yang F, Wang L, Shucheng H, Jiang X. Differences in clinical characteristics of rosacea across age groups: A retrospective study of 840 female patients. J Cosmet Dermatol. 2023 Mar;22(3):949-957. doi: 10.1111/jocd.15470.
- Roster, K., Fleshner, L., Karatas, T.B. et al. Menopause and Common Dermatoses: A Systematic Review. Am J Clin Dermatol (2025). https://doi.org/10.1007/s40257-025-00994-0.
- Emmerson E, Hardman MJ. The role of estrogen deficiency in skin ageing and wound healing. Biogerontology. 2012 Feb;13(1):3-20. doi: 10.1007/s10522-011-9322-y.
- Horng HC, Chang WH, Yeh CC, Huang BS, Chang CP, Chen YJ, Tsui KH, Wang PH. Estrogen Effects on Wound Healing. Int J Mol Sci. 2017 Nov 3;18(11):2325. doi: 10.3390/ijms18112325.
- El Mohtadi M, Whitehead K, Dempsey-Hibbert N, Belboul A, Ashworth J. Estrogen deficiency – a central paradigm in age-related impaired healing? EXCLI J. 2021 Jan 11;20:99-116. doi: 10.17179/excli2020-3210.
- Hirschberg AL. Approach to Investigation of Hyperandrogenism in a Postmenopausal Woman. J Clin Endocrinol Metab. 2023 Apr 13;108(5):1243-1253. doi: 10.1210/clinem/dgac673.
- Atmaca M, Seven İ, Üçler R, Alay M, Barut V, Dirik Y, Sezgin Y. An interesting cause of hyperandrogenemic hirsutism. Case Rep Endocrinol. 2014;2014:987272. doi: 10.1155/2014/987272.
- Viscomi B, Muniz M, Sattler S. Managing Menopausal Skin Changes: A Narrative Review of Skin Quality Changes, Their Aesthetic Impact, and the Actual Role of Hormone Replacement Therapy in Improvement. J Cosmet Dermatol. 2025 Sep;24 Suppl 4(Suppl 4):e70393. doi: 10.1111/jocd.70393.
- Vincent C, Bodnaruc AM, Prud’homme D, Olson V, Giroux I. Associations between menopause and body image: A systematic review. Womens Health (Lond). 2023 Jan-Dec;19:17455057231209536. doi: 10.1177/17455057231209536.
- Pagac MP, Stalder M, Campiche R. Menopause and facial skin microbiomes: a pilot study revealing novel insights into their relationship. Front Aging. 2024 Mar 21;5:1353082. doi: 10.3389/fragi.2024.1353082.